Doctor Appointment App Development Company Guide (2026)
Looking for a doctor appointment app development company? Find expert tips on 2026 costs, features, and tech stacks to build your custom medical app today.

Building a medical app in 2026 feels a lot like fixing a plane mid-flight. You need something fast and reliable, yet it cannot crumble under the weight of strict regulations. Many clinics are still clinging to outdated systems — paper ledgers, basic spreadsheets, phone trees — while their patients quietly wonder why booking a doctor feels harder than ordering a pizza.
The digital health market is not slowing down. Industry analysts estimate it is growing at roughly 17% annually, with projections placing the sector north of $200 billion by 2030. If your practice has not started thinking seriously about a purpose-built app, you are already behind the curve.
This article is for clinic owners, practice managers, and health-tech founders who want a clear-eyed look at what building a medical scheduling app actually involves — from choosing a development partner to understanding compliance requirements and future-proofing your investment.
Choosing a Development Partner
The first and most consequential decision you will make is who builds your software. Some firms are all talk and no substance. They show you slick presentations and case studies from unrelated industries, then struggle to explain what FHIR or HL7 standards even mean. Walk away from those conversations.
A team worth working with will ask smart questions before proposing anything. They will want to understand your existing systems, your patient demographics, how your staff currently manages scheduling, and what compliance obligations you operate under. The quality of their questions tells you more than the quality of their pitch deck.
Teams with experience in mobile app development in Texas, for instance, often bring a strong understanding of regional healthcare regulations while also serving clients with national or multi-state compliance needs. Working with a team grounded in local market realities while operating at a higher technical level is frequently a better fit than chasing the cheapest offshore quote.
When evaluating any development firm, ask directly about their experience handling large medical record databases, their security audit process, and which compliance frameworks they have built against. If their answers are vague, keep looking.
Features Your Patients Will Actually Use
Patients in 2026 do not have patience for clunky interfaces. If your app requires more than a few taps to book an appointment, many of them will simply call a competitor instead. The bar for usability has never been higher.
Telehealth integration has moved from a nice-to-have to a basic expectation. Your app needs a stable video platform — one that does not drop calls halfway through a consultation. Alongside that, virtual triage features can help your staff quickly sort who needs an in-person visit and who can be helped remotely, reducing waiting room crowding and improving patient flow.
Secure messaging and file sharing reduce the volume of phone calls your front desk handles every day. Patients want to send a quick message about a prescription, upload a photo of a rash, or share their insurance card without picking up the phone. That convenience keeps them engaged with your practice.
Automated reminders are perhaps the highest-return feature in the entire app. Clinics that implement well-timed push notifications — one the day before a visit and one an hour before — have reported no-show rates dropping by 25 to 30 percent. That is a direct impact on monthly revenue, and it costs almost nothing to implement once the infrastructure is in place.
Understanding the Real Cost
Cost is always the first question and almost never has a simple answer. A basic MVP scheduling app for a single clinic might cost $50,000 to $80,000 all in. A full-featured platform with EHR integration, AI-assisted documentation, and wearable device connectivity can run significantly higher.
Here is a realistic breakdown by development phase:
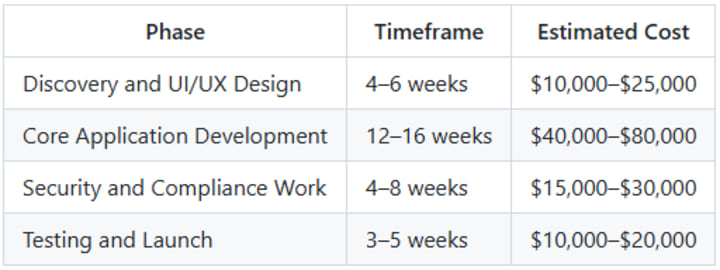
Design is often underestimated. An interface that an 80-year-old patient can navigate without confusion requires dedicated user testing and iteration — not just a competent visual designer. Cutting that budget typically results in higher support costs and lower adoption rates down the line.
Back-end infrastructure is where most of the hidden costs live. Healthcare-grade cloud hosting, ongoing security audits, and compliant data storage are not optional line items you can defer. They are foundational, and they carry recurring costs that your budget should account for year over year.
Compliance Is Not Optional
HIPAA is not a checklist you complete once and forget. It is a framework that needs to be embedded into every layer of your application from the first line of code. How data is stored, who can access it, how it is transmitted, how long it is retained — all of this must comply with federal standards if your app handles protected health information in the United States.
If you have any European users or partners, GDPR adds another layer of obligation. The two frameworks overlap in many areas, but diverge in important ways, particularly around user consent and data deletion rights.
All data in transit must be encrypted, and all data at rest should be protected with a standard like AES-256 — which is effectively the industry floor for medical applications. Your development team should also be able to explain their key management practices clearly. If they cannot, that is a red flag.
What Is Coming Next
The most exciting developments hitting medical apps right now involve generative AI. Tools that listen to a patient-physician conversation and automatically generate a structured clinical summary are already being deployed in some practices. For physicians drowning in documentation, the time savings are significant.
Predictive health alerts — where an app analyzes patterns in a patient's data and flags potential issues before they escalate — are moving out of research settings and into real clinical workflows. These tools do not replace physician judgment, but they give practitioners better information, earlier.
Wearable device connectivity is also expanding rapidly. Your app should be designed with open APIs that can pull data from smartwatches, continuous glucose monitors, and other consumer health devices. Patients managing chronic conditions are increasingly relying on these tools, and a scheduling app that can see that data tells a much fuller story than a ten-minute visit ever could.
Where to Go From Here
Building a medical app is a significant undertaking. There will be difficult weeks, integration headaches, and moments where the compliance requirements feel overwhelming. But when a patient successfully books a life-changing appointment through something your team built — quickly, securely, from their phone — the investment makes complete sense.
Start by clearly defining the problem you are solving. Talk to your staff and your patients before writing a single line of code. Then find a development partner who asks better questions than you do.
The clinics and health organizations that invest thoughtfully in digital infrastructure today are the ones that will be best positioned for the next decade. The tools available are genuinely powerful. The only question is whether you use them.
Frequently Asked Questions
How long does building a medical scheduling app typically take?
Most projects run between four and nine months from kickoff to launch. The wide range reflects how much variation there is in feature scope, integration complexity, and the pace of compliance review.
Is HIPAA compliance required for all medical apps?
Yes, if your application handles protected health information in the United States. Other regions have their own equivalent frameworks — GDPR in Europe being the most prominent. Compliance cannot be added after the fact; it must be designed in from the start.
Can a custom app connect to our existing hospital software?
In most cases, yes. Modern applications use standardized APIs and healthcare interoperability protocols to connect with Electronic Health Record systems. This allows patient data to flow between platforms without requiring manual re-entry.
What feature should we prioritize first?
Easy, fast scheduling is consistently the top priority for patients. If a user can find an available time and confirm a booking in under sixty seconds, you have solved the core problem. Reminders and secure messaging are strong second priorities.






Comments
There are no comments for this story
Be the first to respond and start the conversation.